Advances in Orthopedic Surgery
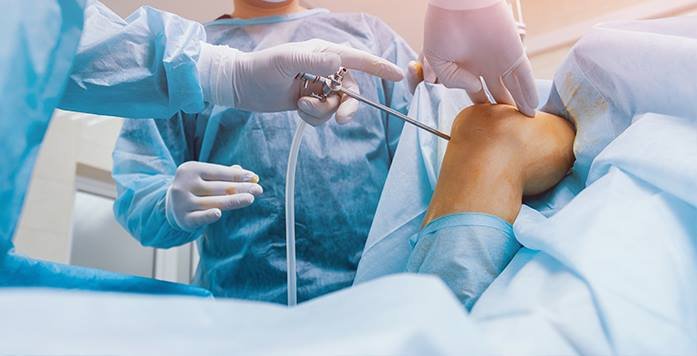
Orthopedic surgery advances include the continuous evolution, refinement, and integration of novel methodology, technology, and therapeutic approaches within the specific domain of orthopedics. This complex evolution entails ongoing research and implementation of cutting-edge surgical procedures, cutting-edge medical technology, and evidence-based practices aimed at treating a wide range of musculoskeletal disorders and injuries.
Orthopedic surgery advances represent a dynamic and interdisciplinary effort to constantly push the boundaries of knowledge, technology, and clinical practice in order to provide cutting-edge care, restore function, and improve the quality of life for people suffering from musculoskeletal ailments and injuries.
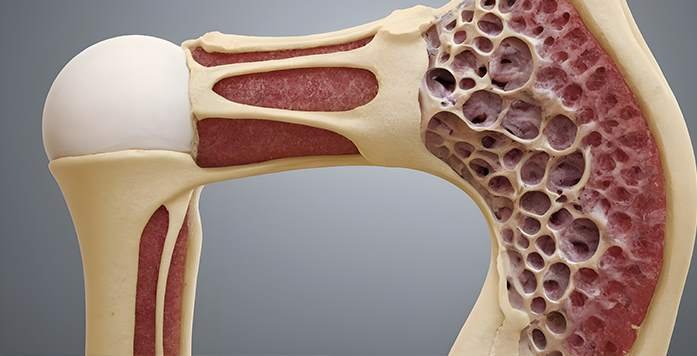
- Bone and Joint Surgery
- Orthopedic and Trauma Surgery
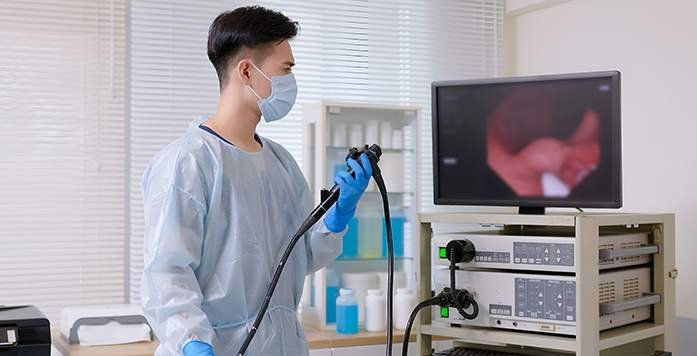
- Arthroplasty, Arthroscopic and Related Surgery
- Shoulder and Elbow Surgery
- Arthroscopic and related surgery
- Hand and Knee Surgery, Sports Traumatology
- Orthopedic and Traumatology Science and Research
- Trauma and Emergency Surgery
- Ankle Surgery, Knee Surgery, Paediatric Surgery
- Trauma Surgery and Other Surgeries
- Hand and upper extremity
- Shoulder and elbow
- Total joint reconstruction (arthroplasty)
- Foot and ankle surgery
- Spine Surgery and Research